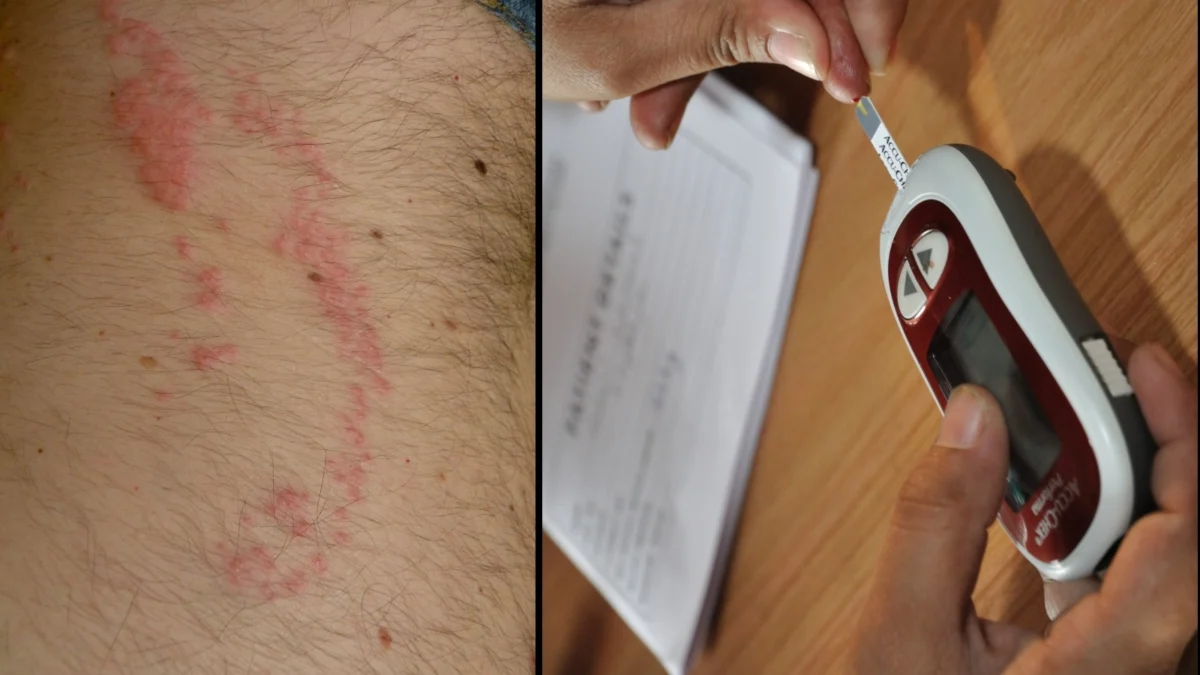
For many, a persistent patch of dry skin, a lingering itch, or a rash that refuses to dissipate begins as an easily ignorable annoyance. It’s often dismissed as a minor allergic reaction or a fleeting dermatological whim. However, a growing body of evidence, amplified by public curiosity and expert insights, suggests that these seemingly innocuous skin changes can, in some cases, be an early and crucial indicator of diabetes. This realization has prompted a deeper exploration into the intricate connection between blood sugar levels and skin health, urging individuals to pay closer attention to their body’s subtle signals.
The burgeoning interest in this topic was recently highlighted on the popular online forum Quora, where a user posed a direct and resonant question: "What does a diabetic skin rash look like?" The sheer volume of engagement with this query underscores a widespread, yet often unaddressed, concern. In response, this article delves into the multifaceted relationship between diabetes and dermatological manifestations, providing comprehensive information and expert guidance.
DISCLAIMER: This article is compiled from publicly available information and insights from medical professionals. It is intended for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare practitioner for any health concerns or before making any decisions related to your health or treatment.
The Intertwined Nexus: How Blood Sugar Impacts Skin Health
The direct correlation between elevated blood sugar levels and skin health is a fundamental principle in understanding diabetic skin manifestations. When glucose levels in the bloodstream remain persistently high, a cascade of physiological changes begins to affect the skin’s integrity and its ability to function optimally.
One of the primary impacts of hyperglycemia is dryness. High blood sugar can disrupt the skin’s natural moisture barrier, leading to a loss of hydration and a feeling of tightness and flakiness. This dryness, in turn, can make the skin more vulnerable to irritation and micro-tears, creating an entry point for pathogens.
Furthermore, chronic high blood sugar can impair blood flow to the extremities. The small blood vessels in the skin, particularly in the legs and feet, can become damaged over time, reducing the delivery of essential nutrients and oxygen. This compromised circulation further hinders the skin’s ability to repair itself and maintain a healthy state.
Perhaps one of the most significant consequences is the weakening of the body’s ability to fight infections. Diabetes can suppress the immune system’s response, making individuals more susceptible to bacterial, fungal, and viral infections. When the skin barrier is compromised by dryness and poor circulation, and the body’s defenses are weakened, the likelihood of developing skin infections and inflammatory responses, such as rashes, significantly increases.
Decoding the Diabetic Rash: Visual Clues and Early Indicators
Distinguishing a diabetic skin rash from a more common dermatological issue can be challenging, as the initial signs are often subtle and easily overlooked. However, understanding the typical presentation and characteristics of these rashes can empower individuals to seek timely medical attention.
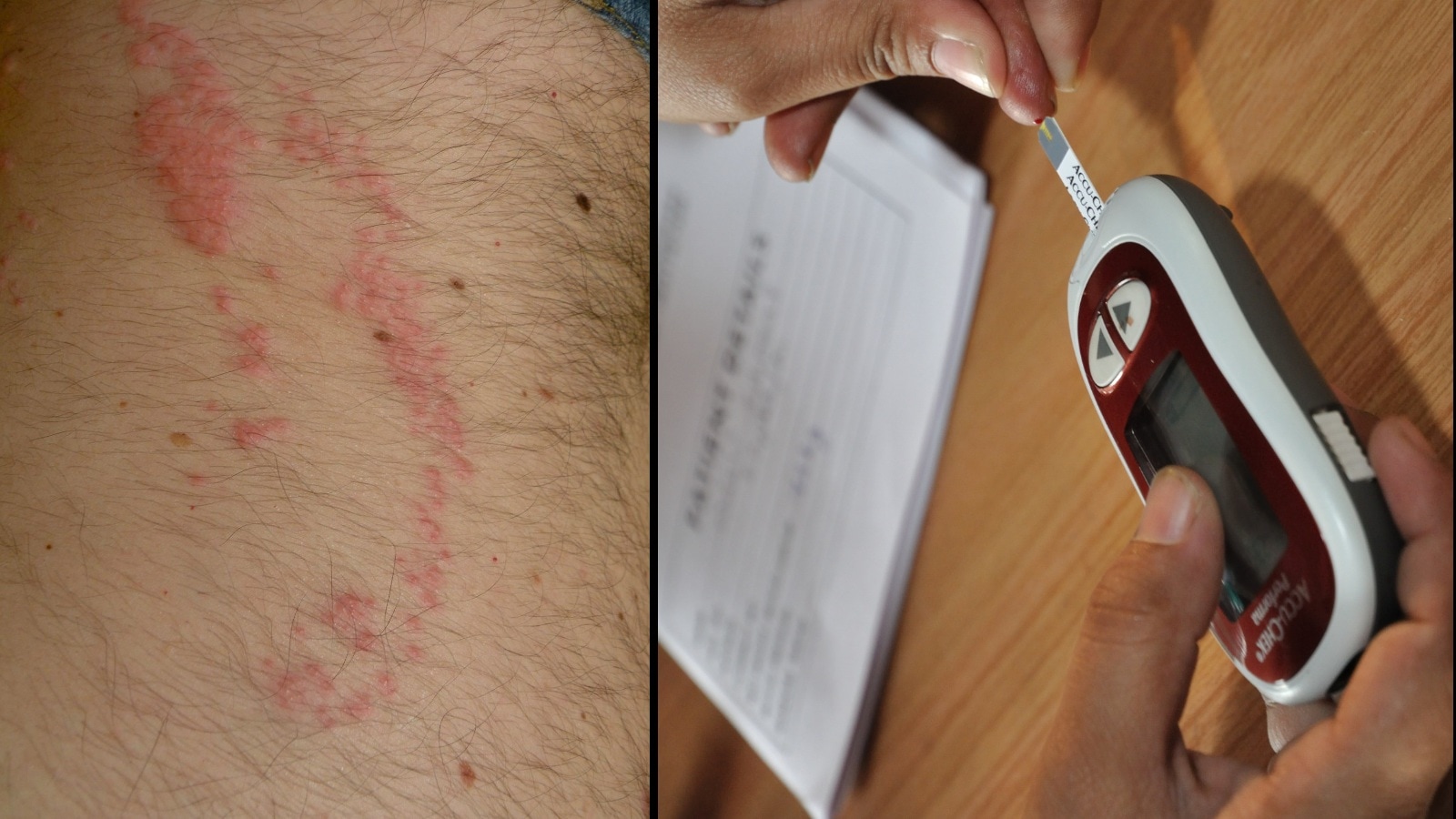
According to Dr. Pankaj Bansal, a Senior Consultant in Internal Medicine at Sharda Care Healthcity, a diabetic skin rash can manifest in several ways. "A diabetic skin rash can appear as dry, itchy, red patches or small brownish spots, usually on the legs, arms, or neck," he explains. These patches may not always be overtly inflamed or painful, contributing to their initial dismissal.
In some instances, individuals with diabetes might notice thickened or darkened skin, a condition known as acanthosis nigricans, which often appears in areas of friction like the neck, armpits, or groin. While not always a rash in the traditional sense, it is a significant skin change linked to insulin resistance, a precursor to type 2 diabetes.
The subtlety of early signs is a critical point. Persistent dryness that doesn’t respond to standard moisturizers, ongoing itching without an apparent cause, or skin changes that take an unusually long time to heal can all be early indicators. These are not necessarily dramatic eruptions but rather a constellation of persistent, bothersome symptoms that deviate from the norm.
Dr. Bansal emphasizes the importance of proactive skin care in the context of diabetes management. "Keeping blood sugar under control is one of the most important steps to maintain healthy skin," he states. This underscores the fundamental principle that managing the underlying condition is paramount to addressing its dermatological sequelae.
Differentiating from Common Rashes: A Matter of Persistence and Pattern
The key distinction between a diabetic rash and a typical allergic reaction or common skin irritation lies in their behavior and response to treatment. While a regular allergy often appears suddenly after exposure to a trigger and resolves relatively quickly with basic remedies, diabetic rashes tend to be more persistent and recalcitrant.
"Diabetic rashes tend to last longer, come back frequently, and may be linked with other symptoms like dryness, infections, or slow healing," Dr. Bansal elaborates. This means that over-the-counter creams or antihistamines that typically alleviate common rashes may prove ineffective, leaving the individual frustrated and the condition unresolved.
The chronicity and recurrence of these rashes are significant red flags. They don’t simply disappear with a change in diet or environment; they often linger, creating a sense of unease and prompting further investigation. The association with other symptoms like extreme dryness, a tendency to develop infections (e.g., recurrent boils or fungal infections), or wounds that heal at a snail’s pace further strengthens the suspicion of an underlying diabetic link.
When to Seek Professional Guidance: Recognizing the Urgency
The decision to consult a healthcare professional should be guided by the persistence, severity, and accompanying symptoms of any skin change. Experts unanimously advise vigilance, particularly when a rash deviates from expected patterns.
A rash that fails to improve within a few days, begins to spread rapidly, becomes increasingly painful, or shows signs of infection such as increased redness, warmth, swelling, or the presence of pus, warrants immediate medical attention. These are clear indicators that the skin is compromised and requires professional intervention.
Dr. Bansal reiterates the critical nature of addressing slow-healing wounds and recurrent infections. "Slow-healing wounds or repeated infections should never be ignored," he stresses. He highlights that diabetes significantly impairs the body’s wound-healing capabilities, increasing the risk of complications, including severe infections that can spread to deeper tissues and even lead to limb amputation in severe cases.
A Spectrum of Skin Concerns: Beyond the Rash
The relationship between diabetes and skin health extends far beyond the scope of a single type of rash. Individuals with diabetes are prone to a variety of dermatological conditions, many of which serve as valuable diagnostic clues.
Fungal and bacterial infections are significantly more common in people with diabetes due to their impaired immune response and the favorable environment created by hyperglycemia for microbial growth. Common culprits include Candida (yeast infections), which can cause itchy rashes in warm, moist areas, and Staphylococcus bacteria, which can lead to boils and carbuncles.
Diabetic dermopathy, also known as "shin spots," presents as light or dark brown, scaly patches, often on the shins. These are thought to be related to changes in small blood vessels in the skin. While generally harmless, they are a visible sign of microvascular complications associated with diabetes.
As previously mentioned, acanthosis nigricans is a distinct sign of insulin resistance and is often seen in individuals with prediabetes or type 2 diabetes. The characteristic dark, velvety thickening of the skin in folds like the neck and armpits is a clear indicator that requires medical evaluation.
Beyond these specific conditions, generalized dryness and itching (pruritus) are pervasive complaints among people with diabetes, particularly when blood sugar levels are poorly controlled. This can be attributed to the cumulative effects of impaired circulation, nerve damage (neuropathy), and altered skin barrier function.
In essence, the skin often acts as a barometer for overall health, and for individuals with diabetes, it can be one of the first places where something feels "off." Paying close attention to persistent and unusual skin changes, especially those that linger or recur, can be a vital step in the early detection and effective management of diabetes and its associated complications.
The Unseen Epidemic: Implications for Public Health
The trending nature of keywords like "diabetic" on search engines like Google in recent times is a testament to the growing public awareness and concern surrounding this chronic condition. This heightened interest, fueled by accessible information and personal experiences shared online, underscores the urgent need for continued public health initiatives focused on diabetes prevention, early detection, and comprehensive management.
The implications of this connection between skin health and diabetes are far-reaching. For individuals, recognizing these subtle skin cues can lead to earlier diagnosis, allowing for timely intervention and the implementation of lifestyle modifications and medical treatments that can significantly improve long-term health outcomes and prevent serious complications.
From a public health perspective, this understanding can inform targeted screening programs and educational campaigns. By highlighting the dermatological manifestations of diabetes, healthcare providers can empower individuals to be more proactive about their health and encourage them to seek medical advice when they notice persistent or unusual skin changes.
The interconnectedness of various bodily systems means that addressing one aspect, such as skin health, can have a ripple effect on overall well-being. Therefore, a holistic approach to healthcare, one that considers the intricate interplay between different organs and functions, is crucial in the fight against diabetes and its myriad challenges.
DISCLAIMER: This article is compiled from publicly available information and insights from medical professionals. It is intended for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare practitioner for any health concerns or before making any decisions related to your health or treatment.